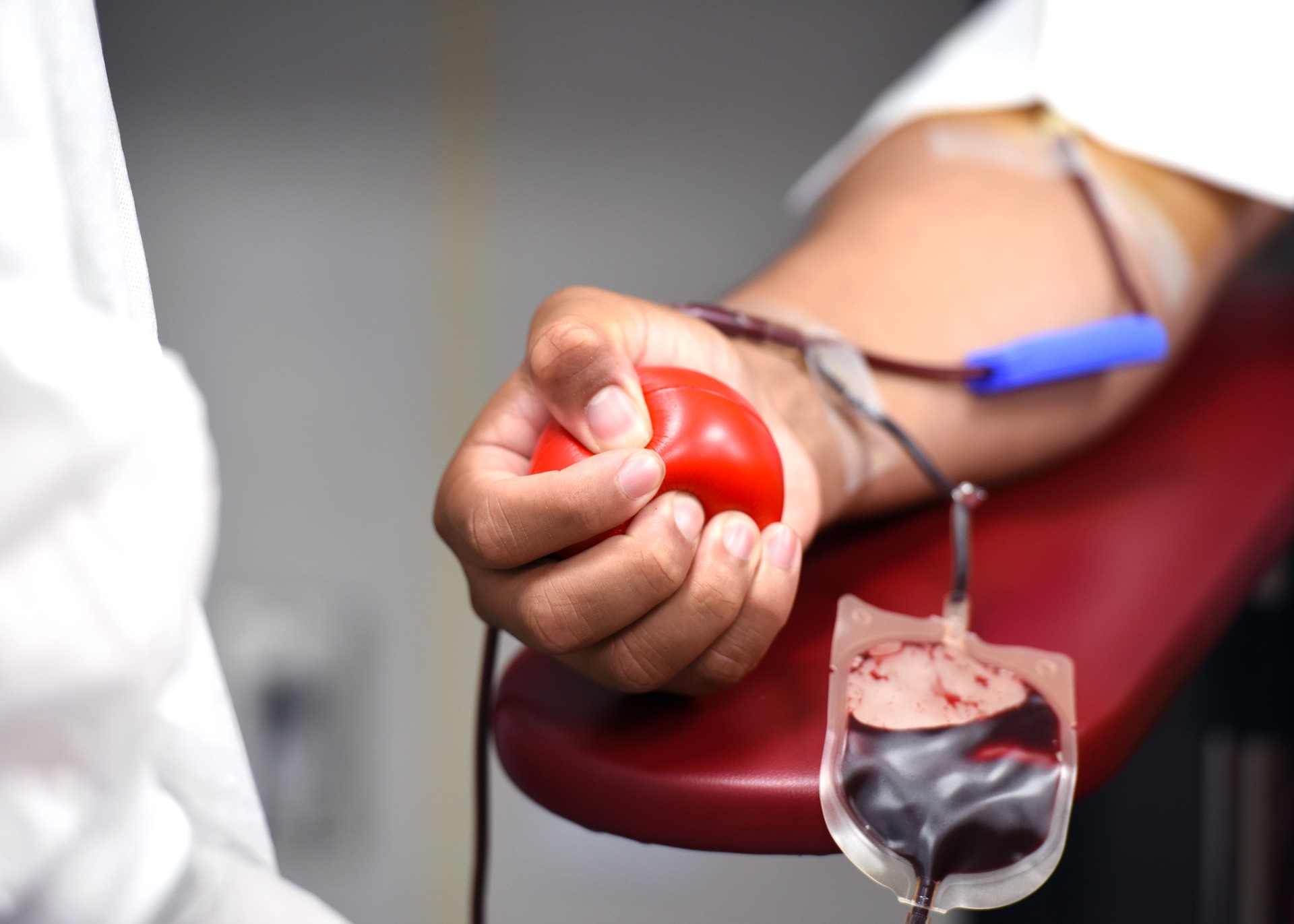
Imagine a distant reality where blood banks carried a seemingly unlimited surplus of blood stocks, tailored to the patient’s condition, all without a drop of donated blood. A game-changing trial launched this month is taking the first strides in this direction by transfusing lab–grown red blood cells (RBCs) into healthy human participants.
If shown to be safe and effective, lab-grown RBCs may offer a new transfusion product to supplement the NHS’ critically depleted blood stocks.
This could provide readily available transfusions for patients with rare blood diseases, including sickle cell anaemia and thalassemia, where the body fails to synthesise enough haemoglobin.
The RESTORE trial (REcovery and survival of STem cell Originated REd cells) is a collaboration between the University of Bristol, NHS Blood and Transplant (NHSBT), and the University of Cambridge. The stocks of RBCs are manufactured from donated adult blood stem cells through a process called “differentiation”.
While previous trials have transfused RBCs differentiated from blood stem cells taken from the same patient, this will mark the first trial where RBCs generated from a donor’s stem cells are to be transfused into an unrelated recipient, a process called “allogeneic transfusion”.
Professor Ashley Toye, Professor of Cell Biology at the University of Bristol and Director of the NIHR Blood and Transplant Unit in red cell products explains during an interview in Bristol,
‘[t]his challenging and exciting trial is a huge stepping stone for manufacturing blood from stem cells. This is the first-time lab grown blood from an allogeneic donor has been transfused’.
The single-blind phase I trial will call for 10 healthy volunteers from Cambridgeshire to receive two mini-transfusions, approximately 10ml of blood each, spaced four months apart.
In an encouraging pilot study to test safety, two volunteers transfused with the manufactured RBCs showed no unexpected side effects or immune shock following transfusion.
Aside from confirming the safety of the transfusion method, the study also hopes to demonstrate that the RBCs manufactured in the lab have a longer lifespan in the body compared to conventional donated blood, which normally lies at around 50–60 days (but varies widely per person).
On reducing the frequency of blood transfusions, the Chief Investigator, Professor Cedric Ghevaert at the University of Cambridge and NHSBT stated in an interview,
‘We hope our lab-grown red blood cells will last longer than those that come from blood donors. If our trial, the first such in the world, is successful, it will mean that patients who currently require regular long-term blood transfusions will need fewer transfusions in future, helping transform their care’.
The researchers hope this technology will particularly benefit patients with specific blood disorders, who might require lifelong blood transfusions ‘because they have an inherited genetic disorder and they can’t make their blood themselves or they make blood cells that do not work as well as they could so they have to be topped up by red cells coming from another source, at the moment these are blood donors’, said Ghevaert.
But further research is required before the results from this trial can represent a therapeutic treatment option for patients.
The challenge facing researchers now is producing more substantive quantities of RBCs from a few teaspoons to around 350ml, as is routinely used in adult blood transfusions.
While RBCs grown in vitro might improve therapies for patients carrying rare blood types or blood diseases, the demand for blood donations will continue, as John Hames OBE, Chief Executive of the Sickle Cell Society, put it,
‘[W]e should remember that the NHS still needs 250 blood donations every day to treat people with sickle cell and the figure is rising. The need for normal blood donations to provide the vast majority of blood transfusions will remain’.